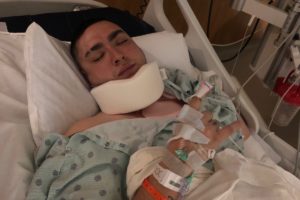
Stamford Veteran Struggles to Pay Medical Bills After Hit-and-Run
Brian Eirin a 28-year-old US Infantry Veteran and father of three is struggling to pay his medical bills after being involved in a hit-and-run accident on January 10th, 2020. He suffered a fractured neck, fractured skull and brain bleed when a car hit his motorcycle from behind, throwing him headfirst ...

TUNNEL TO TOWERS RUN By Robin Isidro
Sunday, September 29th marked the 18th annual Tunnel To Towers 5K run and walk that retraces the steps of FDNY firefighter Stephen Siller, who was on his way home after his shift on Sept. 11, 2001, when he got word of a plane hitting one of the World Trade Center towers ...

2019 BATTLE OF BROOKLYN RUCK MARCH Freedom Isn’t Free – And Boy, Do I have The Blisters To Prove It
By Patrick Dillon If there’s one thing I can’t stand more than sending very young True Believers like me off to fight an unwinnable war with one arm tied behinds our backs, it’s walking. Why? Because ever since I moved almost 30 years ago uptown to Harlem (where my WWII vet Irish-born father was a fireman ...

Why This Marine Teaches Yoga
by Kate Hendricks Thomas, PhD, MCHES I used to think strength meant presenting an image of strong silence and always looking like I had everything together. I was a Marine, a leader, and could never make a mistake. I became a Marine to serve, and loved being part of the ...

Spring Cleaning
By Fatima Cook There’s a freshness in the air! The earlier rising and later setting sun clearly marks the time for a refreshing reset. Time to clean out with what's no longer “sparking joy” (in the words of Marie Kondo) and make space to fill with joie de vivre. Aside from ...

The Impact of Invisibility: Military Veteran Women’s Health
By Kate Hendricks Thomas I still remember being told I should never walk around our base in Iraq alone. Would you believe that it didn’t even seem strange at the time? Today I’m a public health researcher. A big part of what I do is try to figure out how ...

“Transcendental Meditation made me human again. I came back from the dead. I was resurrected.”
By Corey O'Brien Corey O’Brien is a US Army and Ohio National Guard veteran with a TBI and PTSD who credits his recovery to a Transcendental Meditation program for veterans, enabled through a partnership between the Resurrecting Lives Foundation and David Lynch Foundation. O’Brien is a science teacher at Hamilton Township High School ...

Army Veteran and Artist Lt Col David Richardson will Auction His Original Artwork to Benefit Fellow Veterans with PTSD
NEW YORK, NY, MARCH 2019 — Vanity Fair celebrity interviewer George Wayne and Award Winning TV Host and Best Selling Author, Rita Cosby will be co-hosting an exhibition and benefit at The Solider and Sailors Club at 283 Lexington Avenue on Thursday, March 14th @ 6PM.
Wayne will be auctioning off ...
Wayne will be auctioning off ...

Big Shout-Out to SFTT’s Crowd-Funders for Getting Eric to Pocatello for “Treatment of Ten”
by Ben Richards "Why isn't everyone getting this?" was the first question he asked me. Eric and I were talking about his experience going through Stand for the Troop's (SFTT) "Treatment of Ten" program.
Eric served our Nation for more than two decades, through multiple combat deployments and like so many ...
Eric served our Nation for more than two decades, through multiple combat deployments and like so many ...

The Holidays
By Dr. Kate Hendricks Thomas Dr. Kate Hendricks Thomas is the author of Brave, Strong, True: The Modern Warrior’s Battle for Balance and co-author of Bulletproofing the Psyche. As holidays approach, I’m uniquely grateful for the loved ones in my life. I’m also ever-mindful that there’ve been times when I ...

Bulletproofing
by Dr. Kate Hendricks Thomas What if I told you that mental fitness is something you can develop in the same way you build your physical fitness? We hear a lot these days about mental fitness in politics and leadership. When we do, the conversation often focuses on avoiding or ...

MaryAnn H.A. Dyer & Wookiee
My name is MaryAnn H.A. Dyer, I am a Retired, 100% Disabled, female Army Veteran, with a Military Occupational Skill (MOS) in Intelligence (TSBICI). I have Post Traumatic Stress Disorder (PTSD) with Night Terrors, Military Sexual Trauma (MST), Panic Attacks, Fibromyalgia, Degenerative Spine and Severe Migraines. I love the Army ...
